- AI
- Molecular Imaging
- CT
- X-Ray
- Ultrasound
- MRI
- Facility Management
- Mammography
The Rise of NPP Image Interpretation: What New Radiology Research Reveals
In a retrospective review of over 110 million imaging claims for patients with commercial insurance or Medicare Advantage, researchers noted key trends signaling significant increases in imaging billed by non-physician practitioners (NPPs).
Non-physician practitioner (NPP) billing for imaging interpretation reportedly had over a 25 percent overall increase, a greater than 40 percent increase in communities under the national median household income (MHI) and over a 30 percent increase in metropolitan areas between 2016 and 2020, according to newly published research examining 110,649,811 commercial and Medicare Advantage insurance claims for diagnostic imaging.1
For the retrospective study, recently published in Current Problems in Diagnostic Radiology, researchers noted a number of emerging trends with NPP-billed imaging. Here are seven takeaways from the study.
1. While physicians consistently accounted for the vast majority of diagnostic imaging claims over the five-year study period (96.7 percent in 2020), NPP-billed imaging increased from 2.6 percent of the overall imaging billing claims in 2016 to 3.3 percent in 2020. This represents a 26.9 percent increase for NPP-billed image interpretation, according to the study authors.1
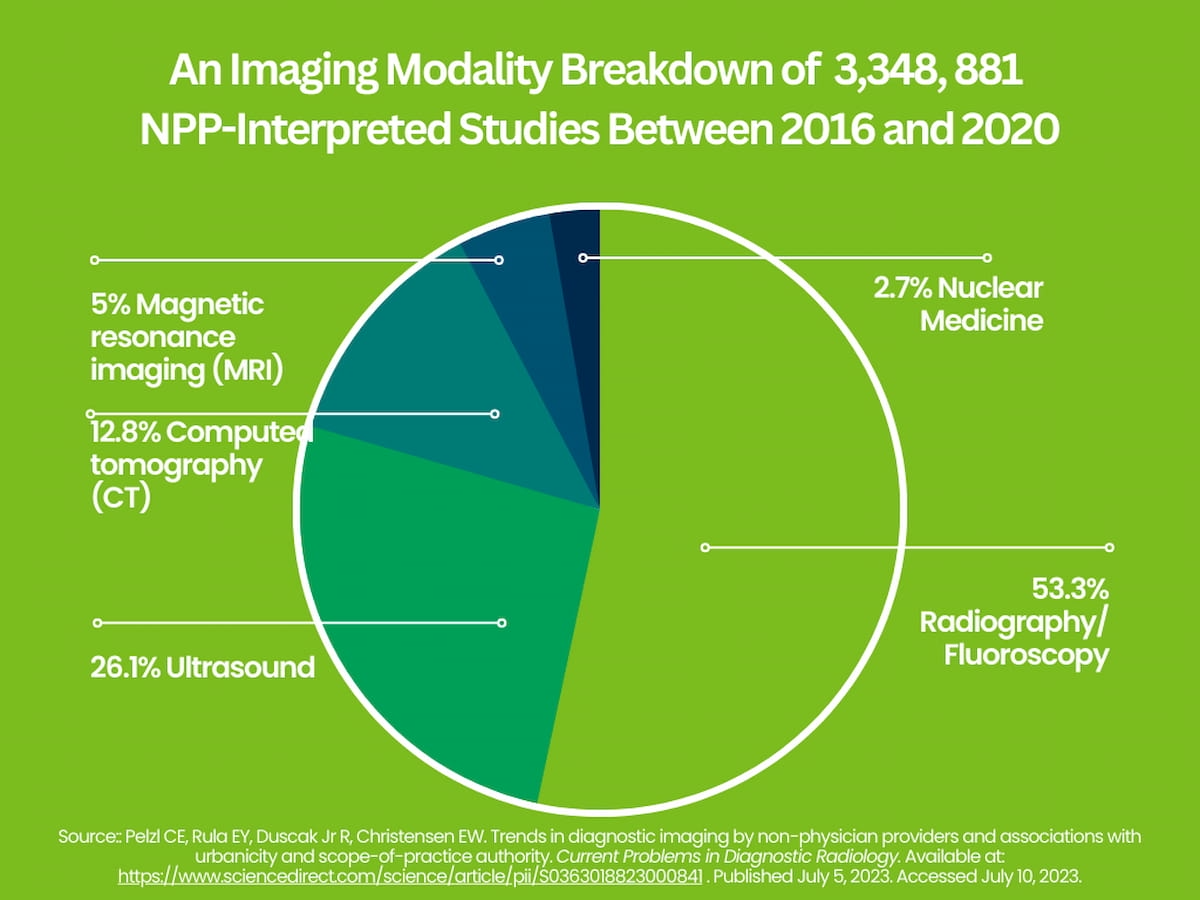
2. Out of 3,348,881 imaging studies interpreted by NPPs during the five-year study period, 53.3 percent were for radiography or fluoroscopy, 26.1 percent were for ultrasound interpretation, 12.8 percent involved computed tomography (CT), 5 percent for magnetic resonance imaging (MRI) reading and 2.7 percent involved nuclear medicine imaging.1
Out of 3,348,881 imaging studies interpreted by NPPs during the five-year study period, 53.3 percent were for radiography or fluoroscopy and 26.1 percent were for ultrasound interpretation.
3. Citing related research, the study authors noted that one survey of nurse practitioners (NPs) found that 75 percent expressed no confidence or being “somewhat confident” in assessing skeletal radiography.2
4. While researchers noted similar overall percentage increases in NPP-billed image interpretation for micropolitan (18.9 percent increase) and small town/rural areas (18.8 percent increase) between 2016 and 2020, they found the largest percentage increase in metropolitan areas (31.2 percent).1
5. In regard to state differences in NPP scope of practice, the researchers found that the largest increase in NPP-billed imaging in metropolitan areas (55.5 percent) occurred in the least restrictive states and the largest increase in micropolitan areas (20.2 percent) occurred in moderately restrictive states. For small town/rural settings, the study authors noted that the largest increase in NPP-billed imaging (67.9 percent) occurred in the most restrictive states.1
6. NPP-billed imaging increased by 40.4 percent from 2016 to 2020 in communities with less than the national MHI. In contrast, the researchers noted that NPP-billed imaging increased by 20.4 percent during that time period in communities with equal or greater than the national MHI.1
7. In regard to place of service, long-term care facilities had the lowest share of NPP-billed imaging in 2020 (7.6 percent) in comparison to outpatient facilities that accounted for 46.6 percent of NPP-billed imaging, according to the study.1
References
1. Pelzl CE, Rula EY, Duscak Jr R, Christensen EW. Trends in diagnostic imaging by non-physician providers and associations with urbanicity and scope-of-practice authority. Current Problems in Diagnostic Radiology. Available at: https://www.sciencedirect.com/science/article/pii/S0363018823000841 . Published July 5, 2023. Accessed July 10, 2023.
2. Kirkland SA, Champion JD. Radiologic imaging content in family nurse practitioner programs: a needs assessment. J Nurse Pract. 2018;14(3):e63-e66.
Leading Breast Radiologists Discuss the USPSTF Breast Cancer Screening Recommendations
May 17th 2024In recognition of National Women’s Health Week, Dana Bonaminio, MD, Amy Patel, MD, and Stacy Smith-Foley, MD, shared their thoughts and perspectives on the recently updated breast cancer screening recommendations from the United States Preventive Services Task Force (USPSTF).
The Reading Room Podcast: Emerging Trends in the Radiology Workforce
February 11th 2022Richard Duszak, MD, and Mina Makary, MD, discuss a number of issues, ranging from demographic trends and NPRPs to physician burnout and medical student recruitment, that figure to impact the radiology workforce now and in the near future.
Multicenter CT Study Shows Benefits of Emerging Diagnostic Model for Clear Cell Renal Cell Carcinoma
May 15th 2024Combining clinical and CT features, adjunctive use of a classification and regression tree (CART) diagnostic model demonstrated AUCs for detecting clear cell renal cell carcinoma (ccRCC) that were 15 to 22 percent higher than unassisted radiologist assessments.
CT Study: AI Algorithm Comparable to Radiologists in Differentiating Small Renal Masses
May 14th 2024An emerging deep learning algorithm had a lower AUC and sensitivity than urological radiologists for differentiating between small renal masses on computed tomography (CT) scans but had a 21 percent higher sensitivity rate than non-urological radiologists, according to new research.