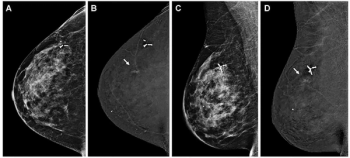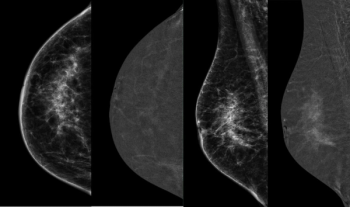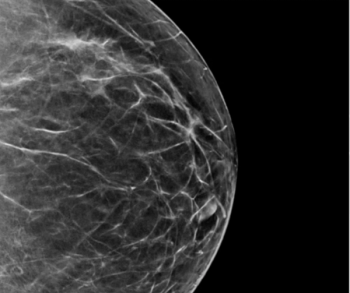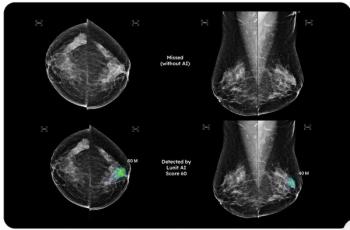
Initial breast cancer risk scoring with adjunctive AI assessment of screening mammograms increased by approximately 80 percent in a subsequent screening round for women with breast cancer, according to research findings presented at the European Congress of Radiology.