What a New CT Study Reveals About Hypoattenuation Thickening After Left Atrial Appendage Occlusion (LAAO) Procedures
The presence of high-grade hypoattenuation thickening on follow-up computed tomography (CT) after left atrial appendage occlusion (LAAO) procedures for patients with atrial fibrillation was associated with a 4.6-fold risk for stroke, according to newly published research.
For patients with atrial fibrillation who undergo left atrial appendage occlusion (LAAO) procedures, the authors of a new study found that high-grade hypoattenuation thickening (HAT) on follow-up computed tomography (CT) was associated with a significantly higher risk of stroke.
For the prospective multicenter study, recently reported in Radiology, researchers reviewed follow-up CT data from 412 study participants (mean age of 76) with atrial fibrillation who had LAAO procedures from January 2012 to November 2020. Follow-up CT exams were performed at a mean of 4.2 months after the LAAO procedure, according to the study.
Low-grade HAT was evident on follow-up CT for 23.8 percent of the cohort and high-grade HAT was found on CTs for 5.1 percent of the study participants. The study authors found that low-grade HAT was associated with a 0.46 odds ratio of persisting left atrial appendage patency but no increased risk of stroke.
Study participants with high-grade HAT were 9.5 times more likely to have antithrombotic drug discontinuation and had a 4.6-fold higher risk of stroke, according to the study authors.
“Distinguishing between low-grade and high-grade HAT seems clinically relevant because the former is associated with a favorable risk profile whereas the latter exposes patients to higher risks that should cause the initiation of preventive measures,” wrote study co-author Hubert Cochet, M.D., Ph.D., an associate professor in the Department of Cardiac Imaging at the University Hospital of Bordeaux in Pessac, France, and colleagues.
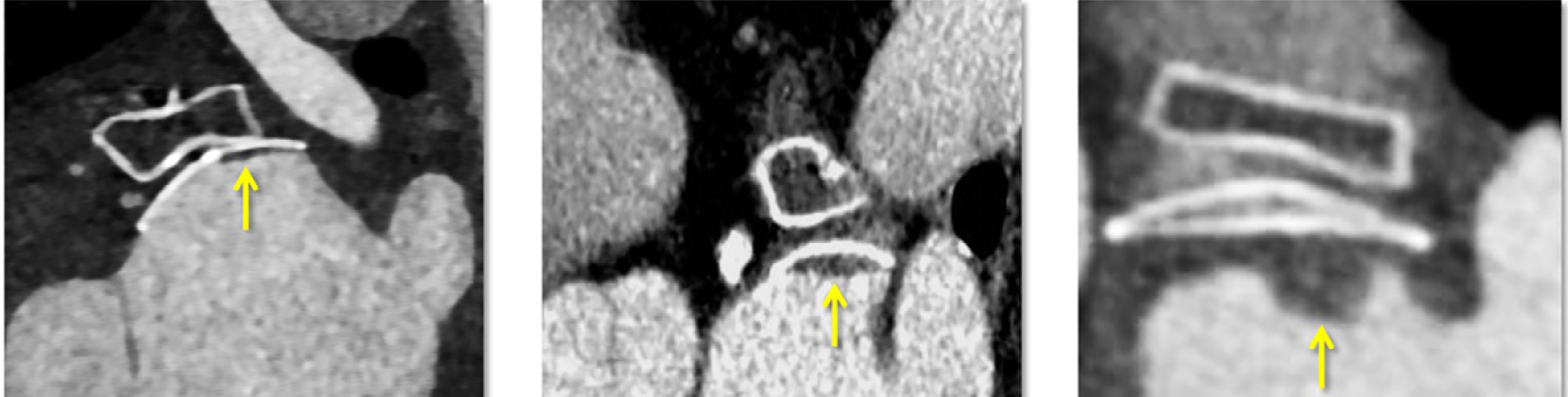
For the analysis of possible hypoattenuation thickening (HAT) associated with pacifier devices for left atrial appendage occlusion (LAAO), the computed tomography (CT) images above show: flat sessile hypoattenuation (< 1 mm) suggestive of endothelialization (left); flat, sessile, low-grade HAT (1-3 mm) (middle); and high-grade HAT (> 3 mm or pedunculated/irregular) (right). (Images courtesy of Radiology.)
Of the 21 patients who had high-grade HAT on CT, the study authors noted that three patients died after the first follow-up CT exam. For the remaining 18 patients treated with either antiplatelet or anticoagulant therapy, Cochet and colleagues pointed out that nine patients had HAT regression at a mean of 84 days after the initial follow-up CT findings.
“These findings support the introduction of unequivocal standardized CT criteria for HAT grading with important implications for treatment regimen optimization after implantation,” added Cochet and colleagues.
(Editor’s note: For related content, see “Study Suggests Benefits of Preoperative CT for Left Atrial Appendage Occlusion Procedures” and “Coronary CT Angiography Study Shows Link Between Major Cardiovascular Events and High Lipid Core Burden”)
In regard to study limitations, the researchers noted a lack of follow-up data for patients with low-grade HAT, which may have factored into the under-diagnosis of late device-related thrombosis (DRT). While LAAO device position reportedly plays a role in DRT formation, the study authors conceded that no analysis specific to device position was performed. Variable delays between LAAO procedures and follow-up CT exams were another limitation of the study, according to the authors.
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.
Study Shows Enhanced Diagnosis of Coronary Artery Stenosis with Photon-Counting CTA
July 10th 2025In a new study comparing standard resolution and ultra-high resolution modes for patients undergoing coronary CTA with photon-counting detector CT, researchers found that segment-level sensitivity and accuracy rates for diagnosing coronary artery stenosis were consistently > 89.6 percent.
Can CT-Based Deep Learning Bolster Prognostic Assessments of Ground-Glass Nodules?
June 19th 2025Emerging research shows that a multiple time-series deep learning model assessment of CT images provides 20 percent higher sensitivity than a delta radiomic model and 56 percent higher sensitivity than a clinical model for prognostic evaluation of ground-glass nodules.