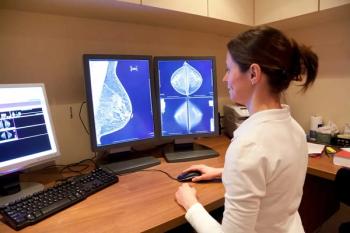
Digital Breast Tomosynthesis Cuts Recall Rate
Digital breast tomosynthesis plus mammography provides a 40 percent reduction in patient recalls, reducing anxiety and potentially cutting cost and overall radiation dose.
Digital breast tomosynthesis plus mammography screening provides a 40 percent reduction in patient recalls, say researchers from Yale University School of Medicine in New Haven. The results of their study were presented at the American Roentgen Ray Society Annual Meeting in Vancouver, Canada.
Recalls can be very stressful for the women, and the recall rate following traditional 2-D mammography alone is 11.1 percent, researchers said. To evaluate if recalls were fewer when combining screening, researchers compared that rate with the rate for women who underwent both a mammogram and digital breast tomosynthesis.
The recall rate following both a mammogram and digital tomosynthesis was only 6.6 percent, researchers found.
When women had masses, the recall rate was similar, but the recall rate was significantly lower when women had the screenings together, compared to mammography alone, for asymmetries (2.8 percent versus 7.1 percent, respectively) and calcifications, said Melissa Durand, MD, one of the study authors.
Liane Philpotts, MD, another study author, explains why: “
The radiation dose for the two exams is below both the dose of film mammography and the FDA limit for mammography. The goal is to be able to get all the required information from just the tomosynthesis, eliminating the need for the 2-D mammogram, researchers said.
Not only do fewer recalls reduce the anxiety caused for the women involved, researchers said, but they also provide a cost savings and may reduce the
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.