ER Imaging Study Looks at Possible Complications of COVID-19 Vaccines
Lung opacities/consolidation and cervical/axillary adenopathy are reportedly common findings in emergency room imaging of patients suspected of having complications related to COVID-19 vaccines, according to new research presented at the American Roentgen Ray Society (ARRS) conference.
In new research presented today at the 2022 American Roentgen Ray Society (ARRS) Annual Meeting, the authors of a new emergency room (ER) imaging study found that lung opacities/consolidation and cervical/axillary adenopathy were common imaging findings in patients who presented with symptoms such as chest pain and shortness of breath after recent COVID-19 vaccination.
For the study, which took place between December 2020 and August 2021, the authors reviewed 168 radiology reports on 173 studies for 161 patients (mean age of 47 years) who presented to the emergency room with symptoms ranging from chest pain and headache to shortness of breath and cough after recent vaccination for COVID-19. The researchers noted that 57.7 percent of the radiology reports demonstrated no evidence of vaccine-related complications. In the remaining 42.3 percent of reports that showed positive findings, 36.6 percent of these reports revealed lung opacities/consolidation and 35.2 percent showed cervical and/or axillary adenopathy, according to study co-author Margarita Revzin, MD, MS, FAIUM, an Associate Professor of Radiology and Biomedical Imaging at the Yale University School of Medicine, and colleagues.
While the researchers assessed a variety of imaging in this study population, chest X-ray (39.3 percent) and CT chest angiography (10.4 percent) were the most ordered tests, which was consistent with chest pain (27 percent) and shortness of breath (17 percent) being the most common symptoms of patients in the study. Other symptoms of patients presenting to the ER included headache (12.5 percent), cough (11.9 percent) and fever (10 percent).
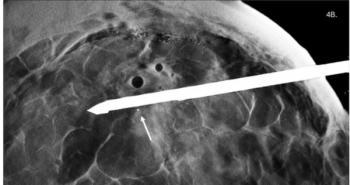
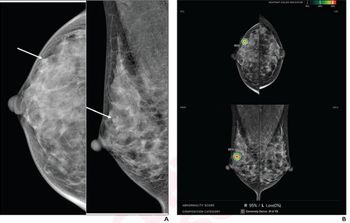
Some of the cases included in the authors’ online poster presentation at the ARRS conference included the development of septic arthritis 20 days after vaccination in a 77-year-old man; saddle pulmonary embolus and residual deep vein thrombosis in a 30-year-old woman four days after vaccination; and left axillary lymphadenopathy three days after a second vaccination in a 16-year-old male.
The study authors acknowledged study limitations including variability between the patient presentation to the ER and the time of vaccination, data being limited to a single center, and reference to recent vaccination in imaging reports to identify relevant studies for inclusion in the study.
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.