Focus on Smokers, Patients With Negative Lung CTs to Improve Lung Cancer Screening Adherence
Concentrating on current smokers and those without positive CT results can improve patient participation and cost effectiveness.
Despite the recommendations that smokers get screened for lung cancer, not all patients at risk for the disease actually do so. And, identifying who those patients are can maximize the efficacy of programs designed to screen for lung cancer, a recent study reported.
Concentrating lung cancer screening efforts on patients still smoking or individuals who have negative low-dose lung CT scans is the best way to increase the utility of screening initiatives, said researchers from the University of Pennsylvania Perelman School of Medicine in an article published in the
“When devising interventions to augment lung cancer screening adherence, it is crucial to focus on negative exams and on current smokers,” said the team led by Eduardo J. Mortani Barbosa Jr., assistant professor of radiology at the Hospital of the University of Pennsylvania. “Radiologists must be creative and proactive in implementing solutions.”
Even though low-dose CT lung cancer screenings have been shown to decrease mortality, existing research shows that getting people to stick with routine screening can be difficult. Getting a better understanding of why some people adhere to the programs and why some fall off can ultimately make these initiatives not only more clinically effective, but more cost-effective, as well.
Related Content:
“Our study confirms that smoking behavior does not change for most lung cancer screening persons even following multiple rounds of lung cancer screening,” he pointed out, “and that a more concerted and intensive effort at encouraging smoking cessation is necessary during shared decision-making.”
The Study
To determine the real-world effectiveness of low-dose lung CT screenings, Barbosa’s team conducted a retrospective study with 260 participants who returned for follow-up screening between 2014 and 2019. At baseline, 55 percent were current smokers, up from 46.5 percent who had been current smokers at their previous screening. The team recorded patient demographics, smoking history and behavior changes, Lung-RADS category, positive- and negative-predictive value, and their adherence to screening recommendations.
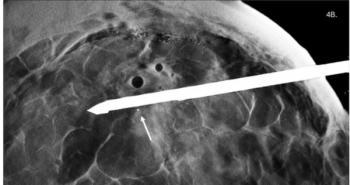
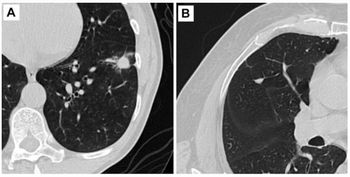
According to their study analysis, 43 patients – 16.5 percent – had positive low-dose CT scans. Of that group, 28 people (10.8 percent) were a Lung-RADS Category 3; eight people (3.1 percent) had Category 4A, six (2.3 percent) were 4B, and 2 (0.8 percent) were 4X. Four of the participants received cancer diagnoses – three lung cancers and one metastatic melanoma.
The overall adherence rate, Barbosa’s team determined, was 43 percent, but the rate was higher among patients with higher Lung-RADS scores. In addition, former smokers were also more likely to stick with the screening program that were current smokers, 50 percent versus 36.2 percent, respectively. Based on these evaluations, the team determined adherence was overwhelmingly influenced by two factors – previous smoking history and a Lung-RADS category of equal to or greater than 3.
Bolstering Screening Adherence
There are ways, though, that radiologists can improve patient adherence to lung cancer screening protocols, Barbosa said.
For example, providers can create automated electronic medical record tracking systems that can detect patients who miss their lung cancer screening appointments. Attaching an economic incentive, such as health insurance premium reductions, to continued participation can also be effective.
Augmented communication efforts can also play a critical role, he said. Multi-modal communication that includes in-person conversations with radiologists and referring providers, as well as letters and electronic reminders should be examined as possible strategies. In those cases, communications should specifically and clearly point out one factor that can be critical to patients sticking with the program.
“Such communications should emphasize that a negative lung cancer screening exam does not confer immunity to future lung cancer development,” he said, “and that continued participation in lung cancer screening, combined with smoking cessation, is essential to accrue the maximum benefits of mortality reduction amongst persons with substantial smoking history.”
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.