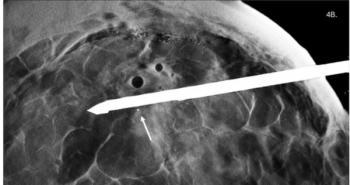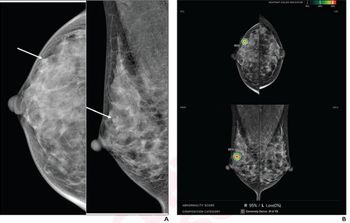
High BMI and Frequency of Breast Cancer Screening
The effect of high BMI on breast cancer screening frequency.
More frequent breast cancer screening may be necessary for women with high body mass index (BMI), according to a study to be presented at
Researchers from Sweden sought to identify risk factors associated with tumors not being detected until they were larger than 2 centimeters and to examine the implications for long-term prognosis.
The researchers examined a population-based screening cohort of 2,358 cases of invasive breast cancer incident between 2001 and 2008; 2,012 patients were followed until 2016. The researchers estimated the multiple adjusted odds ratios for the association between percent density (PD), BMI and other patient characteristics, and the main outcome. Disease progression was defined as the first of locoregional relapse, distant metastasis, or death due to breast cancer.[[{"type":"media","view_mode":"media_crop","fid":"64507","attributes":{"alt":" Fredrik Strand, MD","class":"media-image media-image-right","id":"media_crop_5718862648305","media_crop_h":"0","media_crop_image_style":"-1","media_crop_instance":"8249","media_crop_rotate":"0","media_crop_scale_h":"0","media_crop_scale_w":"0","media_crop_w":"0","media_crop_x":"0","media_crop_y":"0","style":"height: 229px; width: 150px; border-width: 0px; border-style: solid; margin: 1px; float: right;","title":" Fredrik Strand, MD","typeof":"foaf:Image"}}]]
The results showed with screen-detected cancers, both BMI and PD were associated with having a large tumor at diagnosis but for interval cancers, only BMI was associated with having a large tumor. Percent density was associated with having a small tumor. Nulliparity was only significant among screen-detected cases and large tumors were associated with worse prognosis than smaller tumors.
"Our study suggests that when a clinician presents the pros and cons of breast cancer screening to the patient, having high BMI should be an important 'pro' argument," study co-author Fredrik Strand, MD, a radiologist at the Karolinska University Hospital in Stockholm, said in a release. "In addition, our findings suggest that women with high BMI should consider shorter time intervals between screenings."
Strand’s research will continue as he studies how breast density is associated with delayed detection, however his longer-term vision includes the use of artificial intelligence to triage mammographic screening examinations based on breast cancer risk and potential tumor detectability.
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.