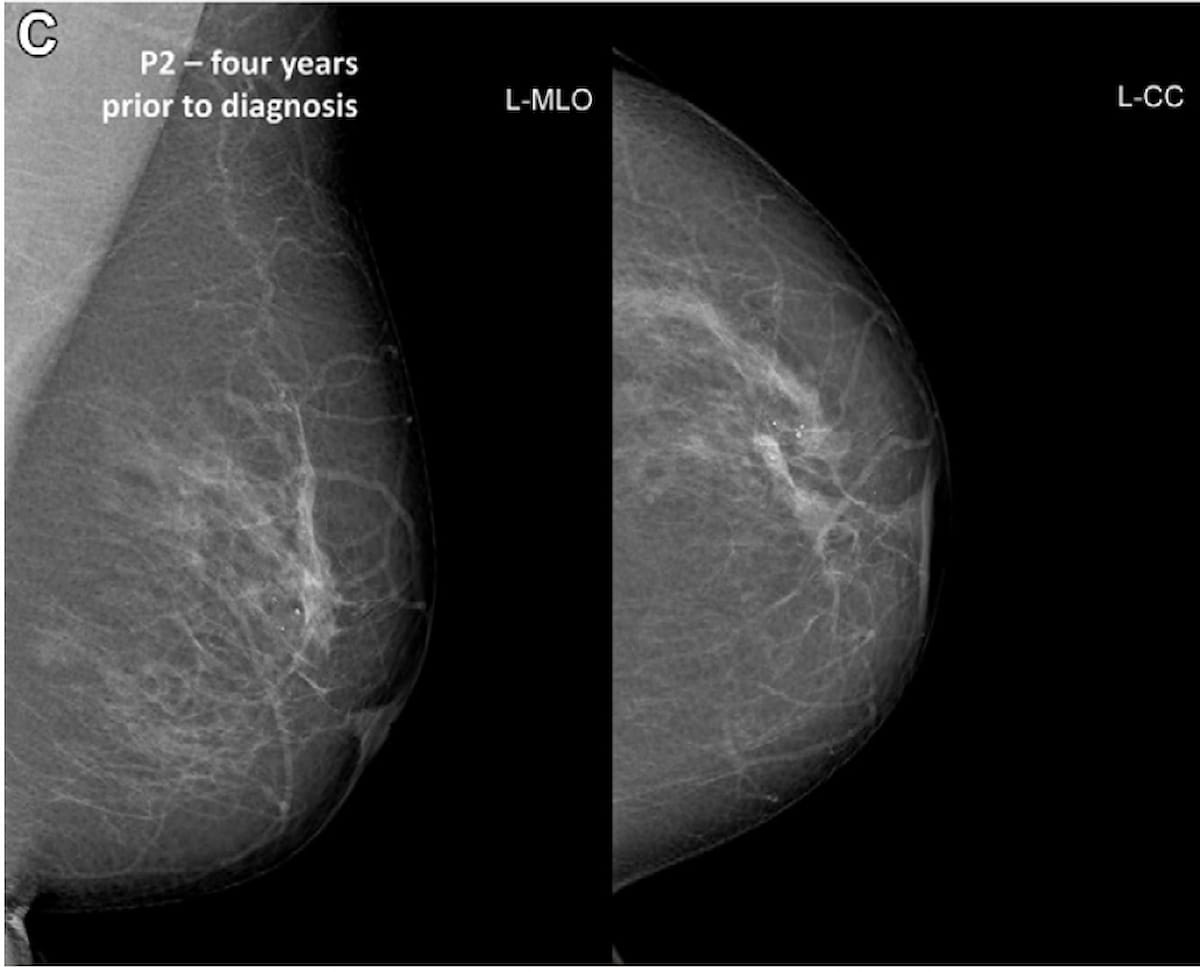
Emerging research suggests that adjunctive use of artificial intelligence (AI) in mammography screening accurately identifies high malignancy risk up to two years prior to diagnosis in over a third of women with screen-detected or interval cancers.
For the retrospective study, recently published in Radiology, researchers evaluated the use of the adjunctive AI software Transpara version 1.7.0 (ScreenPoint Medical) for mammography exams conducted prior to diagnosis in 1,016 patients with screen-detected breast cancer and 586 patients with interval breast cancer. Based on mammographic features, researchers utilized the AI software to assign high-risk (10), intermediate risk (8-9) and low risk (1-7) scores for potential malignancy, according to the study.
For mammography exams conducted two years or less prior to screen-detected breast cancer, researchers found that the AI software assigned a high-risk malignancy score of 10 for 38.3 percent of these cases. For mammograms completed up to two years prior to diagnosis of interval breast cancer, the AI software noted a high risk for malignancy in 39.4 percent of these cases.
“ … We found that more than one in three cases of screen-detected and interval cancers had an artificial intelligence (AI) risk score of 10 at prior screening. This indicates a potential of AI to detect breast cancer earlier, which could lead to less harmful treatment for the affected female patients,” wrote study co-author Solveig Hofvind, Ph.D., who is affiliated with the Section for Breast Cancer Screening of the Cancer Registry of Norway and a professor in radiography at the Oslo and Akershus University College of Applied Sciences in Oslo, Norway, and colleagues.
The study authors also noted that 23 percent of screen-detected breast cancer cases and 23.4 percent of interval breast cancer cases were identified as being at high-risk for malignancy at mammography exams conducted up to four years prior to diagnosis.
Three Key Takeaways
- AI's potential for early detection. The study shows that AI software can accurately identify high malignancy risk in mammography exams conducted up to two years prior to breast cancer diagnosis in over 38 percent of screen-detected cancer cases and over 39 percent of interval cancer cases. This indicates AI's potential to aid in early breast cancer detection.
- Importance of AI risk scores. High-risk AI scores of 10, particularly in combination with calcifications, were associated with an increased likelihood of detecting relevant cancers. This suggests that AI risk scores can help identify cases that may require closer assessment and lead to earlier cancer detection.
- Study limitations. It's important to consider the study's limitations, including the use of only one vendor for mammography exams and the study cohort being limited to women from Norway. Extrapolating the findings to a broader population may be challenging, and further research is needed to explore the correlation between cancer location and AI markings.
In comparison to women with low-risk AI scores of 1 to 7 in the screen-detected breast cancer cohort, the researchers pointed out that calcifications alone or the combination of calcification with breast density were more prevalent among women who had high-risk AI scores.
For mammography exams conducted up to two years prior to diagnosis of screen-detected cancer, density with calcifications was noted in 13.6 percent of patients with AI scores of 10 in comparison to 4.7 percent of patients with AI scores of 1 to 7. The researchers found that 15.8 percent of patients with high-risk AI scores had calcifications alone in contrast to 7.8 percent of those who had low-risk AI scores.
“It might be important to recall women with calcifications and a score of 10 for assessment because it may lead to earlier detection of relevant cancers,” noted Hofvind and colleague. “However, the proportion of calcifications and an AI score of 10 among disease-free women also must be explored because it might influence the rate of false-positive screening results (recalled with a negative result).”
(Editor’s note: For related content, see “Mammography-Based Deep Learning Model Facilitates Higher Breast Cancer Detection on Screening MRI,” “Large Mammography Study Suggests AI is Equivalent to Radiologists for Double Reading of Exams” and “Mammography News: FDA Clears AI Software for Breast Arterial Calcification Detection.”)
In regard to study limitations, the authors noted that only one vendor was used for mammography exams and the study cohort, comprised of women from Norway, may limit extrapolation of the study findings to a broader population. The researchers conceded that a lack of clarity on the correlation between cancer location and AI markings may have impacted the study findings.