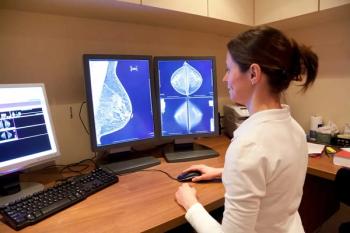
Mammography Improves Cancer Detection, But Triggers More Biopsies
Shifting from film to digital technology for diagnostic mammography has improved cancer detection, and increased the abnormal interpretation rate.
Digital technology has improved cancer detection rates for diagnostic mammography, but has also increased false positive rates, resulting in more biopsies, according to a new study published in
Researchers from Vermont, Washington, California, North Carolina, New Hampshire, Illinois, and Massachusetts sought to establish contemporary performance benchmarks for diagnostic digital mammography with use of recent data from the Breast Cancer Surveillance Consortium (BCSC).
The researchers obtained data from 401,548 examinations conducted among 265,360 women in six BCSC registries. Mammogram indication and assessments were prospectively collected for women undergoing diagnostic digital mammography and linked with cancer.
“Our goals in this study were to produce benchmarks that individual radiologists and breast imaging facilities can use to compare with their own practices and to convey trends in how the metrics have changed over the past 10 to 15 years,” lead author Brian L. Sprague, PhD, from the University of Vermont Cancer Center in Burlington, said in a release.
The results showed cancer detection rate rose from 25.3 per 1,000 in 2005 to 34.7 per 1,000. Other findings included:
• Abnormal interpretation rate: 12.6%
• Positive predictive value (PPV) of a biopsy recommendation (PPV2): 27.5%
• PPV of biopsies performed (PPV3): 30.4%
• False-negative rate: 4.8 per 1,000
• Sensitivity: 87.8%
• Specificity: 90.5%
Among the cancers detected:
• 63.4%were stage 0 or 1 cancers
• 45.6% were minimal cancers
• Mean size of invasive cancers was 21.2 mm
• 69.6% of invasive cancers were node negative
The performance metrics varied widely across diagnostic indications and the cancer detection rate was 64.5 per 1,000. The abnormal interpretation rate was highest for diagnostic mammograms obtained to evaluate a breast problem with a lump (18.7%). Compared with performance during the screen-film mammography era, diagnostic digital performance showed increased abnormal interpretation and cancer detection rates and decreasing PPVs, with less than 70% of radiologists within acceptable ranges for PPV2 and PPV3.
“The results of the study highlight specific areas where quality improvement initiatives should focus,” Sprague said in the release. “Overall, there is a lot of good performance out there, but there are definitely areas for improvement in positive predictive value and abnormal interpretation rate.”
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.