MRI Shows Focused Ultrasound May Induce Immunological Response in Alzheimer’s Patients
Images reveal ultrasound therapy can effectively open and close the blood-brain barrier, opening the door for potential new Alzheimer’s treatments.
Focused ultrasound may be used to ignite an immunological healing response in patients with Alzheimer’s disease – and MRI can help providers see the results.
Based on the results of a first-in-kind clinical trial from West Virginia University (WVU), investigators from WVU School of Medicine and the Rockefeller Neuroscience Institute (RNI) showed that ultrasound can effectively cross the blood-brain barrier to target the hippocampus. They published their results recently in
“The blood-brain barrier has long presented a challenge in treating the most pressing neurological disorders,” said Ali Rezai, M.D., RNI executive director and principal investigator of the clinical trial. “The ability to non-invasively and reversibly open the blood-brain barrier in deep brain areas, such as the hippocampus, offers a new potential in developing treatments for Alzheimer’s disease.”
This is where focused ultrasound comes in, said Rashi Mehta, M.D., associate professor of neuroradiology at WVU.
“Focused ultrasound is an innovative technique and new way of approaching brain diseases, including Alzheimer’s disease,” she said. “Novel technique are needed for Alzheimer’s disease since traditional approaches have not proven effective.”
In this trial, Mehta’s team used ultrasound to target the hippocampus because of the integral role it plays in learning and memory. They enrolled three women – ages 61, 72, and 73 – who had early-stage Alzheimer’s disease and underwent three ultrasound treatments. Each therapy session, conducted at two-week intervals, used a 220-kHz transducer to open the blood-brain barrier and administer a micro-bubble contrast agent that focused on the hippocampus and entorhinal cortex.
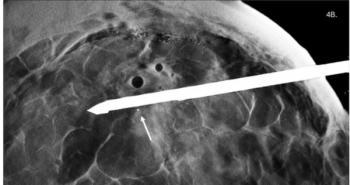
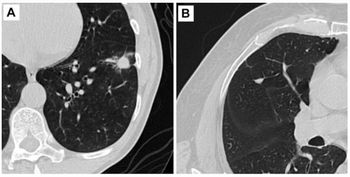
Using 3.0T MRI with gadolinium-enhancement dye, the team saw the changes that took place post-treatment in each patient’s brain. The images revealed the dye moving along the course of draining veins after each procedure. According to their analysis, the MRI images clearly showed the post-procedure contrast enhancement within the targeted brain volumes, indicating treatment had created an immediate, precise blood-brain barrier opening. In addition, they said, parenchymal enhancement was resolved within 24 hours after treatment, confirming that the blood-brain barrier had re-sealed.
It is important to note, she said, that the treatment produced no negative effects. Additionally, the team did not use any medication in this clinical trial – the ultrasound treatment was enough, by itself, to prompt a possible immunological response.
“This imaging pattern was unexpected and enhances our understanding of brain physiology,” Mehta explained. “The glymphatic system, which is a fluid-movement and waste-clearance system that’s unique to the brain, has been studied in animals, but there is controversy about whether this system truly exists.”
The imaging pattern they discovered, she said, not only supports the contention that the system exists in humans, but also that focused ultrasound may be able to modulate the system’s fluid movement patterns and immunological responses. Their evaluation of the MRI findings also points to a possible immunological healing response around the draining veins after the procedure.
“This observation may be an important clue in understanding the physiological mechanism by which the focused ultrasound procedure modifies brain amyloid levels and might be used to treat patients with Alzheimer’s disease and other brain disorders,” she added.
Work within the trial is still ongoing. Ultimately, Mehta said, the team wants to be able to assess whether focused ultrasound can reduce amyloid plaque build-up in patients with Alzheimer’s disease. The next step is to enroll more participants and look at the treatment’s long-term effects, examining its safety and efficacy for slowing – or potentially reversing – the progression of the disease.
For more coverage based on industry expert insights and research, subscribe to the Diagnostic Imaging e-Newsletter
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.