Emerging research from a multinational study involving over 40 facilities reveals a significant degree of variability with the quality of imaging for prostate multiparametric magnetic resonance imaging (mpMRI) exams.
For the multicenter study, recently published in Radiology, researchers utilized the PI-QUAL scoring system to assess 355 mpMRI exams performed at 41 facilities in 18 countries from September 2021 to August 2022.
Out of a total of 71 MRI scanners, the researchers found that only 23 scanners (32 percent) achieved a PI-QUAL score of 5 for optimal imaging quality. According to the study, 39 scanners (55 percent) had a PI-QUAL score of 4 for sufficient image quality and nine scanners (13 percent) had a PI-QUAL score of 3 for sufficient MRI quality.
For the 48 scanners that did not have optimal PI-QUAL scores, the researchers pointed out that dynamic contrast-enhanced (DCE) sequences demonstrated the least adherence to version 2.1 of the Prostate Imaging Reporting and Data System (PI-RADS 2.1). This was evident for 44 of the 48 scanners (92 percent), according to the study authors. The researchers also noted questionable PI-RADS 2.1 adherence in diffusion-weighted imaging (DWI) for 20 scanners (42 percent) and T2-weighted imaging for 19 scanners (40 percent).
“Good image quality has been shown to improve the ability to detect prostate cancer, the accuracy of staging decisions, upstaging after radical prostatectomy, and decision-making for nerve sparing during radical prostatectomy,” wrote lead study author Francesco Giganti, M.D., Ph.D., who is affiliated with the Departments of Radiology and Urology at the University College London Hospital NHS Foundation Trust in London, and colleagues.
“ … Thus, the clinical implications of the study are that centers with diagnostic or treatment services for prostate cancer should take part in quality improvement projects with the aid of quality evaluation systems such as PI-QUAL to optimize their MRI quality and produce clinically useful images for their patients.”
(Editor's note: For related content on prostate cancer imaging, click here.)
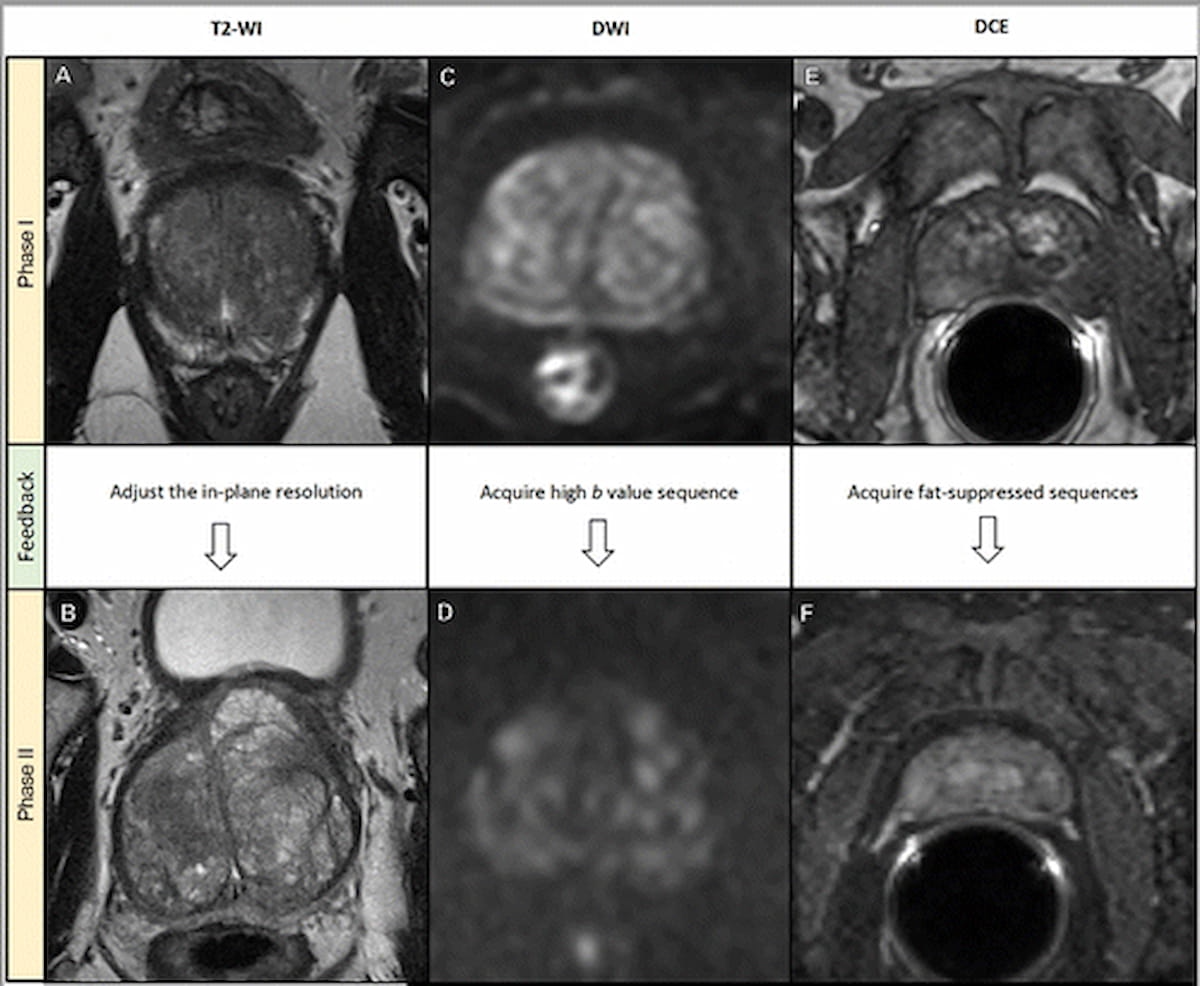
In the second phase of the study, researchers provided feedback to centers that did not achieve optimal PI-QUAL scoring. The most common recommendations for improvement for prostate MRI imaging were as follows:
• adjusting temporal resolution to a maximum of 15 seconds for DCE imaging (56 percent);
• inclusion of an acquired/calculated high b value of greater than 1400 sec/mm2 for DWI sequences (40 percent)
• utilizing fat suppression sequences for DCE imaging (33 percent); and
• adjusting in-plane resolution as per PI-RADS 2.1 guidelines for T2-weighted imaging (21 percent).
Three Key Takeaways
- Variability in prostate MRI quality. The study highlights a significant degree of variability in the quality of imaging for prostate multiparametric magnetic resonance imaging (mpMRI) exams across different facilities and countries, with only 32 percent of MRI scanners achieving the highest PI-QUAL score of 5 for optimal imaging quality.
- Importance of image quality for prostate cancer diagnosis and staging. Good image quality in prostate MRI is crucial for the accurate detection of prostate cancer, making staging decisions, and aiding in surgical planning. The study emphasizes that improvements in image quality can impact clinical decisions and patient outcomes in the management of prostate cancer.
- Quality improvement through feedback. The research suggests that providing feedback and recommendations for improvement to centers with suboptimal MRI quality can lead to significant enhancements in the quality of scans. Adjustments in temporal resolution, high b values for DWI sequences, fat suppression techniques, and adherence to PI-RADS guidelines can contribute to improved image quality.
“After centers received feedback and modified their MRI sequences, we observed a clear improvement in the overall quality of scans across the majority of centers in the study with 97% of the scans at the end of phase II reaching a PI-QUAL score of 5,” added Giganti and colleagues.
(Editor’s note: For related articles, see “Seven Takeaways from Recent Review on Prostate MRI Imaging Quality,” “Can a Deep Learning Algorithm Enhance Detection of Prostate Cancer Recurrence with Biparametric MRI?” and “Study: ‘All Men with PSAs Between 3 and 20 ng/mL Should Undergo MRI Before Biopsy’”)
In regard to study limitations, the researchers suggested that clinicians from those centers that participated in the study may have had a more academic approach to imaging, which may have led to a baseline MRI quality beyond what one may see in routine clinical practice. Noting that the PI-QUAL scoring system used in the study is limited to assessment of mpMRI, Giganti and colleagues suggested that modifications to PI-QUAL would be necessary in order to apply to biparametric MRI if that emerges as a standard of care.