In a study involving nearly 1,000 patients who had head and neck computed tomography angiography (CTA) exams after presenting to the emergency department (ED) with non-focal neurologic complaints, researchers found that 75 percent of the cases were negative, and 7 percent of patients had findings that were unrelated to the original complaint.
For the retrospective study, recently published in the Journal of the American College of Radiology, researchers reviewed data from head and neck CTA exams performed for 960 patients (mean age of 50) who presented to the ED for non-focal neurologic complaints. None of the patients had any history of trauma, recent surgery, or intracranial malignancy, according to the study. The researchers categorized the patients into four groups:
3: acute or emergent findings that may have caused the presenting complaint
2: non-acute or non-emergent findings that may have caused the presenting complaint
1: chronic findings unrelated to the presenting complaint
0: negative findings
The researchers found that only 5.5 of cases involved category 3 findings and 12.5 percent of cases had category 2 findings. Seven percent of the CTA exams revealed findings unrelated to the presenting complaint (category 1) and 75 percent of the cases had no actionable findings at all (category 0), according to the study authors.
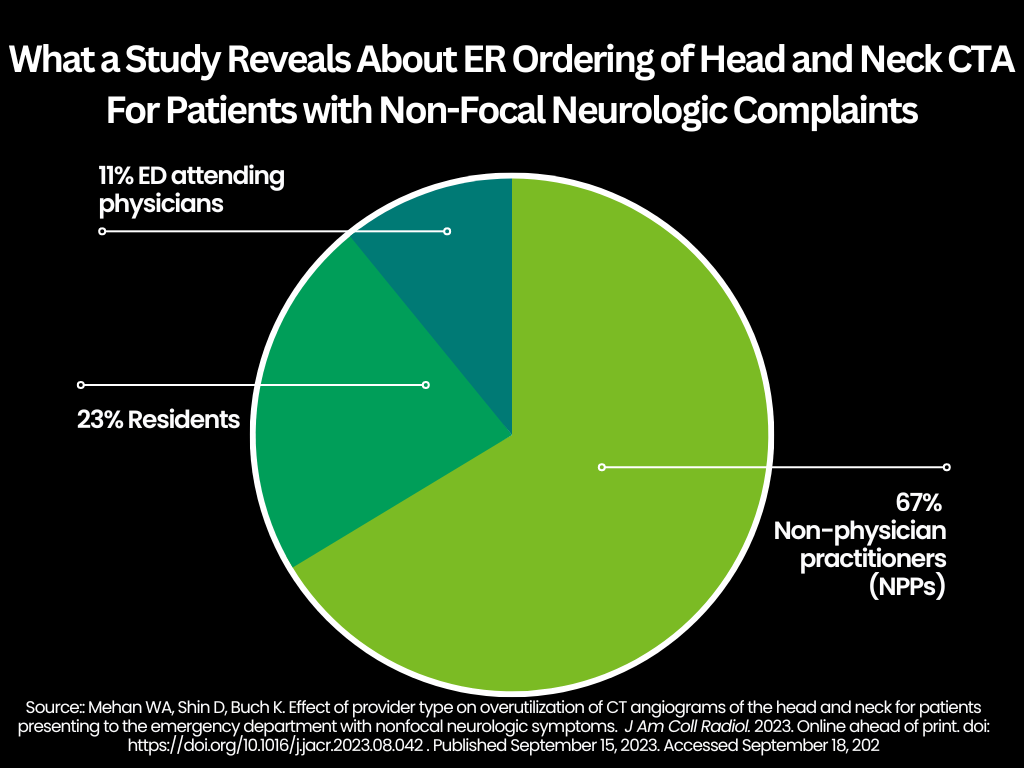
The study authors also found that non-physician practitioners (NPPs) ordered 67 percent of the CTA exams (639 patients), residents ordered 23 percent of the imaging (216 patients) and attending ED physicians ordered 11 percent of the CTA exams (105 patients).
“The results of this study demonstrate that low-yield imaging was performed by ED practitioners at all levels of training,” wrote study co-author Karen Buch, M.D., who is an Associate Professor of Radiology at Harvard Medical School, and colleagues. “However, relatively decreased rates of negativity were seen with more experienced providers, such as the ED department attendings. This suggests that experience of the ED practitioner may influence the utilization of advanced imaging. … This is salient since there is a national trend towards increased NPPs caring for ED patients.”
Three Key Takeaways
1. High incidence of unnecessary imaging. The study highlights that over 80 percent of head and neck CT angiography (CTA) exams performed in the emergency department (ED) for patients with non-focal neurologic complaints had no actionable findings. This suggests a significant overutilization of imaging in this patient population, potentially leading to unnecessary radiation exposure and healthcare costs.
2. Non-physician practitioners (NPPs) ordering imaging. The research found that 67 percent of the CTA exams were ordered by non-physician practitioners (NPPs), such as nurse practitioners or physician assistants. This emphasizes the need for improved education and guidelines for NPPs regarding appropriate imaging utilization to reduce low-yield imaging.
3. Variability in ordering practices. Experienced ED attendings were less likely to order low-yield imaging compared to NPPs. This suggests that the experience and training level of the healthcare provider can influence the appropriateness of advanced imaging orders.
Buch and colleagues found that in comparison to CTA exams ordered by NPPs, CTA exams ordered by ER attendings or residents were 117 percent more likely to reveal severity findings of category 2 or higher. Exams ordered by attending ER physicians were 195 percent more likely to detect high severity scores and CTA exams ordered by resident physicians were 81 percent more likely to show high severity in comparison to CTA exams ordered by NPPs, according to the study authors.
“Future multidisciplinary education efforts coupled with additional imaging-ordering support platforms should be explored to address this pattern and reduce variability in ordering imaging studies,” added Buch, who is affiliated with the Department of Radiology at the Massachusettes General Hospital in Boston, and colleagues.
(Editor’s note: For related content, see “Practical Insights on CT and MRI Neuroimaging and Reporting for Stroke Patients,” “Emergency Department Radiology: Study Shows Higher Imaging Orders by NPPs” and “Is CT Imaging Overutilized in the ER?”)
Noting that there were dedicated CT and MRI scanners in the emergency department at the single level one trauma and level one stroke center where the study took place, the researchers conceded the study results may not apply to a broader population of patients. With the exception of acute code stroke patients, the study authors acknowledged the lack of a standard workup algorithm for patients with neurological deficits at their facility. Required radiologist approval of MRI exams may have been a contributing factor for increased ordering of CTA studies, according to the researchers.