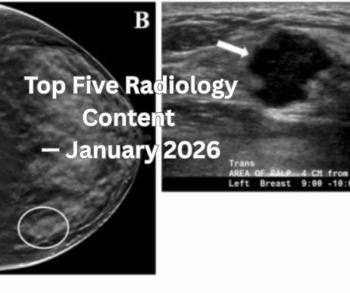
Study scores breast cancer imaging techniques for high-risk women
A small study from a breast cancer surveillance program of high-risk women found that annual MR imaging did not detect additional cancers beyond conventional screening with both mammography and clinical physical examination.
A small study from a breast cancer surveillance program of high-risk women found that annual MR imaging did not detect additional cancers beyond conventional screening with both mammography and clinical physical examination.
Researchers at the University of Dresden evaluated screening surveillance for 41 women with a history of breast or ovarian cancer who had were genetically at risk for breast cancer (carrying the BRCA1 or BRCA2 germ line, for example).
In presenting the study at the ECR on Friday, Dr. Petra Viehweg, a radiologist at Dresden, cautioned that the results are preliminary and the trial numbers were small.
From 5% to 10% of cancers are related to genetic predisposition, and cancers found in these women have a faster growth rate. Women at high risk can undergo prophylactic mastectomy, but this is an invasive, risky option. The majority opt instead for surveillance with imaging.
The Dresden study compared sensitivity and specificity for various techniques: mammography, clinical examination, MRI, and ultrasound. Participants included 32 women with a history of breast cancer, eight with history of ovarian cancer, and one who had previously had both types of cancer. Their median age was 51 years.
The protocol was a clinical examination every six months by a clinician, mammography every year after the age of 30, ultrasound every six months, and MRI every year.
Images were read prospectively and reviewed independently by two radiologists.
Eight lesions were detected. Four were invasive cancers, and one was a high-risk atypical ductal hyperplasia. Of the invasive cancers, three were found on clinical examination (75%), two on mammography (50%), four by ultrasound (100%), and four by MRI (100%). Tumor stage was pT1b in two cases and pT2 in the other two cases. Most cancers were poorly differentiated.
The detection rate in the study group was high at 10%, and the biopsy ratio was acceptable at 1:1, malignant versus benign. Mammography had a high false-negative rate.
Although MRI has not yet shown a benefit for detecting additional cancers, the results could improve as the program continues and a larger number of participants are assessed, Viehweg said.
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.