Study: Combination of Ultrasound and MRI-Targeted Biopsy Enhances Detection of Prostate Cancer
In a study of 413 men with suspected prostate cancer, researchers found the combination of ultrasound and multiparametric MRI-targeted biopsy with systematic biopsy diagnosed prostate cancer in 72.9 percent of patients in comparison to 60.2 percent with systematic biopsy alone.
Emerging research suggests that employing ultrasound and multiparametric MRI-targeted biopsy with systematic biopsy may offer better detection of prostate cancer than systematic biopsy alone.
For the prospective, randomized multicenter study, published recently in Radiology, researchers assessed the use of multiparametric magnetic resonance imaging (MRI) in 582 men (mean age of 65) with suspected prostate cancer (PCa). The study authors also compared the combination of ultrasound and MRI fusion-targeted biopsies with systematic biopsy versus systematic biopsy alone for diagnostic accuracy in prostate cancer imaging.
For 89 men who had positive MRI findings and had a laparoscopic radical prostatectomy, the researchers found that multiparametric MRI successfully identified 131 out of 182 foci with clinically significant prostate cancer (csPCa). In addition to a sensitivity rate of 72 percent, multiparametric MRI had a 71 percent specificity rate and a positive predictive value (PPV) of 78 percent, according to the study. The researchers pointed out that MRI diagnosed 87 percent of cancers with a Gleason score (GS) greater than 7 and 54.4 percent of cancers with a GS of 7.
When comparing the combination of ultrasound and MRI-targeted biopsy along with systematic biopsy versus systematic biopsy alone, the study authors found the combination biopsy had a 12.7 percent higher detection of PCa (72.9 percent vs. 60.2 percent) and 11.4 percent higher detection rate for csPCa (62.8 percent vs. 51.4 percent). Targeted biopsy also offered improved detection of PI-RADS 5 (82 percent vs. 76 percent) and PI-RADS 4 lesions (35 percent vs. 28 percent) in comparison to systematic biopsy alone, according to the researchers.
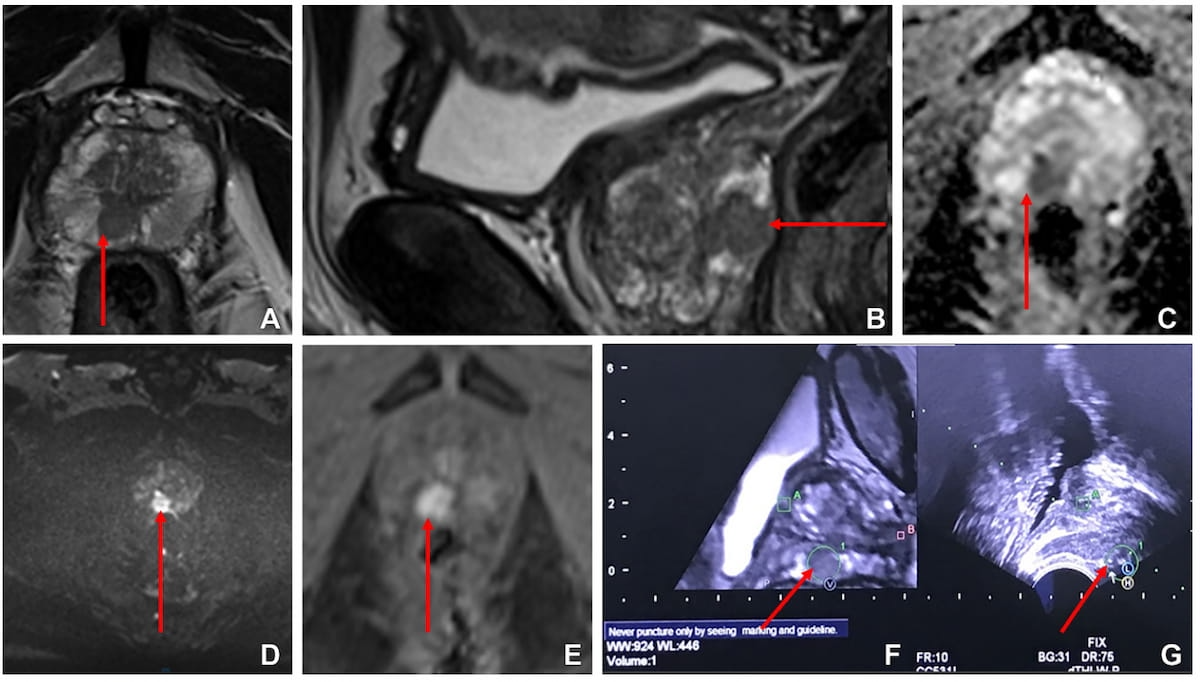
The imaging reveals a focal lesion in the right peripheral zone of the prostate at the mid-gland level in a 60-year-old male study participant. (Images courtesy of Radiology.)
“Although there is still debate regarding the optimal biopsy technique in men without biopsy and with lesions suspicious for cancer at MRI, combined systematic and targeted biopsies for PI-RADS 4 or 5 scores are superior to targeted or systematic biopsies alone in detecting csPCa,” wrote Ghulam Nabi, M.D., a clinical professor in the Division of Imaging Science and Technology at the School of Medicine at the University of Dundee in Dundee, United Kingdom, and colleagues.
Noting challenges with template biopsies and GS grading, the researchers suggested that future research with transcriptomic and radiomic data could enhance a clinician’s understanding of disease grading with intralesional patterns. Nabi and colleagues also emphasized the anterior gland as a potential source of csPCA that was commonly missed in the study.
“The majority of the missed csPCa lesions were smaller than 15 mm and located in the anterior half of the gland,” added Nabi and colleagues. “This observation will be useful for the reporting radiologist to include the anterior gland as a focused review area.”
In regard to study limitations, the researchers noted a lack of interobserver variability among pathologists. They also utilized PI-RADS 2.0 to assess multiparametric MRI findings during the course of the study to help ensure consistency but acknowledged that the updated PI-RADS 2.1 became available in 2019.
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.
Multinational Study Reaffirms Value of Adjunctive AI for Prostate MRI
June 16th 2025The use of adjunctive AI in biparametric prostate MRI exams led to 3.3 percent and 3.4 percent increases in the AUC and specificity, respectively, for clinically significant prostate cancer (csPCa) in a 360-person cohort drawn from 53 facilities.