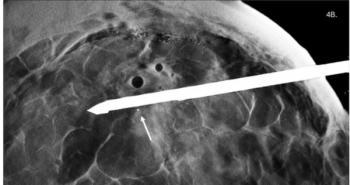
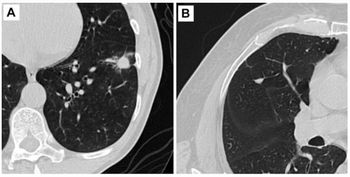
DR products vary markedly in dose and image quality
Buying an expensive digital radiography unit does not guarantee top-notch images or major reductions in x-ray dose. Even more disturbing, some of today's high-priced units can't match the performance of yesterday's discontinued models.The wide variance
Buying an expensive digital radiography unit does not guarantee top-notch images or major reductions in x-ray dose. Even more disturbing, some of today's high-priced units can't match the performance of yesterday's discontinued models.
The wide variance in DR performance was highlighted at this year's European Congress of Radiology. Researchers from Leiden University Medical Center in the Netherlands presented a comparison of effective dose and image quality from eight DR units being used for chest exams in clinical practice.
"Little is known about the clinical implementation of DR," said lead author Wooter Veldkamp, Ph.D., a physicist at Leiden University Medical Center. "Large differences between systems' clinical performance may exist."
Veldkamp and colleagues traveled to five separate hospitals in the Netherlands to conduct their study. DR technologies included in the trial included storage phosphor (Fuji's FCR 5000R with 35 x 43-cm plates), the selenium-coated drum (Thoravision by Philips Medical Systems), scanning CCD (Thorascan by Delft Imaging Systems), optically coupled CCD technology (Swissray's ddR Combisystem), direct selenium TFT (thin-film transistor) (DR 1000C by Hologic), indirect cesium iodide TFT (Siemens' Thorax FD, Philips' Digital Diagnost), and gadolinium dioxide sulphide TFT (Canon's CXDI 40G).
Calculations of each system's effective dose for a chest radiograph for an average patient (height 170 cm, weight 70 kg) were based on entrance dose measurements on an anthropomorphic phantom. For image quality, the team used a contrast detail test object in combination with a phantom that simulated x-ray transmission scatter through the lung. Six such images were acquired from each DR unit. These were then analyzed onscreen by independent observers.
Effective dose varied widely, ranging from 0.009 mSv to 0.028 mSv for the direct readout detectors and hitting 0.033 mSv for the storage phosphor system. The scanning CCD (0.023 mSv) and selenium drum (0.026 mSv) systems came out on top in the contrast detail analysis, showing image quality substantially superior to the other six units, especially the storage phosphor setup.
"The work shows that if you are buying a digital system for chest radiography, it doesn't mean that you are guaranteed optimal image quality. There is still a wide difference in image quality between the DR systems," said Prof. Koos Geleijns, Ph.D., coauthor of the research.
But purchasing decisions are never influenced solely by technical test evaluations, he said. The results, therefore, cannot be regarded as a buyers' guide.
"It is true that the storage phosphor system had the worst image quality in this study and the highest dose, but this technology is cheap, and it can be used at the patient's bedside, which is not so easy with the other systems. So it does have some advantages," Veldkamp said.
By the same token, the selenium-coated drum system ranked at the top for quality, but the technology is far heavier and less maneuverable than TFT flat panels, which also operate at a lower dose. These factors may temper radiologists' disappointment on discovering that the high-performing Thoravision is actually no longer on the market.
Radiologists should quiz vendors that sell low-dose TFT units on how they optimize radiation exposure values, Veldkamp said. Raising the dose slightly will bring image quality into line with the top-performing DR systems in the technical test.
Ultimately, however, getting the most from a DR system may depend as much on the user as the manufacturer's spec.
"With DR, dose can vary more widely than it can in conventional radiography-and image quality can be improved with postprocessing," Veldkamp said. "We can't pinpoint one factor that explains the difference in clinical performance. It is a combination of things."
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.