Understanding Breast Imaging Features of Transgender Women Is Key to Improving Care
Feminizing hormone therapy may increase the risk of breast cancer in transgender women, a growing body of research suggests, underscoring a need for health care providers to understand the risks, breast imaging features, and health care needs of this demographic.
Understanding the potential for breast cancer in transgender women can help health care providers recommend appropriate screening, get a timely diagnosis, and reduce health care disparities among this vulnerable population, a recent review concluded.
The review, published in
“Transgender women commonly use hormone therapy. Although data are limited, there is growing evidence that hormone therapy increases the risk of developing breast cancer compared to cisgender men,” authors Lauren Green, M.D., assistant professor of clinical radiology, and Thomas Lienhoop, M.D., diagnostic radiology resident of the University of Illinois told Diagnostic Imaging.
The study called for development of consistent screening guidelines for transgender women, along with increased awareness of the relevant imaging features and special health care needs to improve care and reduce disparities.
“We were surprised to find there were several conflicting guidelines for breast cancer screening in transgender women, likely because these guidelines are based on expert opinion informed by limited data,” Green and Lienhoop said.
Limitations of existing data include small sample sizes, short duration of follow-up and variable dose and duration of hormone therapy.
The American College of Radiology and the Society of Breast Imaging published
The review noted a variety of hormone therapies that many transgender women continue for life, facilitating breast development and other physical changes such as body fat redistribution, decreased muscle mass, and decreased terminal hair growth.
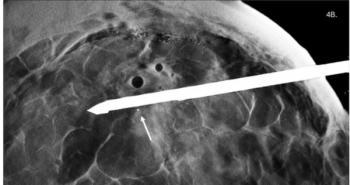
The review highlighted eight case reports of fibroadenoma in transgender women, suggesting that these benign breast tumors might be more common in transgender women than in cisgender men because of hormone use and breast development.
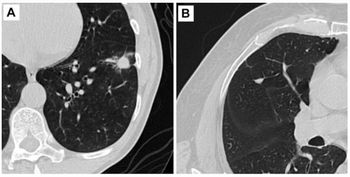
While breast cancer among transgender women is rare, the review noted multiple case reports. The most commonly reported cancer is invasive ductal carcinoma. Conditions with elevated estrogen levels have been associated with increased risk for breast cancer in cisgender men. Studies finding an increased risk for breast cancer in women taking estrogen for five or more years suggest transgender women taking feminizing hormone therapy also may be at increased risk for breast cancer after four or five years.
Breast augmentation surgery is common among transgender women and should be taken into consideration for imaging, which could include implant-displaced views and screening for silicone implant rupture. The review also noted four published cases of breast implant-associated anaplastic large cell lymphoma among transgender women.
“More research with large cohorts and long-term follow-up is needed to characterize the nature of breast cancer and risk of hormone therapy in transgender women,” Green and Lienhoop said. “Because breast cancer is relatively rare in this group, further research may benefit from a centralized database or multicenter trials compiling populations.”
Health care providers also should consider health care disparities faced by transgender women related to stigma, discrimination and lack of access.
“Providers can help address disparities by ensuring their practices are safe and inclusive and by familiarizing themselves with the specific health care needs of this group,” Green and Lienhoop said.
Previous studies have highlighted a need to improve transgender women’s access to competent and compassionate care.
A
A team of experts led by Hannah Perry, M.D., a diagnostic radiologist with the University of Vermont Medical Center, recently published six steps to help radiologists provide the best care possible to this group, including making the office welcoming, asking about pronouns, creating gender-neutral spaces and a comfortable exam environment, improving radiology education and implementing sensitivity.
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.