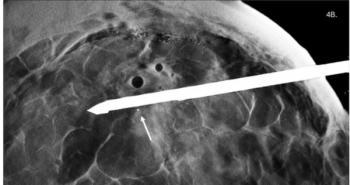
Mammography's 'mortality paradox' resurfaces amid doubts
The merits of screening mammography have again become a subject of debate following new research suggesting that breast cancer surgery speeds up disease progression in young women. The study's authors recommend that breast screening consent forms include the risk of accelerated tumor growth and early relapse.
The merits of screening mammography have again become a subject of debate following new research suggesting that breast cancer surgery speeds up disease progression in young women. The study's authors recommend that breast screening consent forms include the risk of accelerated tumor growth and early relapse.
This latest claim is based on data from 1173 women who underwent mastectomy alone as treatment for breast cancer at the Milan Cancer Institute in Italy between 1964 and 1980 (Int J of Surg 2005;3[3]:179-187). On examining the historic data, researchers noted a significant relapse peak eight to 10 months after surgery. The peak affected 20% of premenopausal patients with node-positive disease. A second, broader relapse peak occurred across the group after five years.
The researchers suggest that the first peak's surprising sharpness is due to a sudden awakening of dormant cancer cells. In other words, the surgical treatment induced angiogenesis. They support the theory with additional calculations showing that their model fits mortality figures and relapse patterns in screening trial data.
"We originally thought that the two different peaks represented two different states of tumors: one dormant and one growing," said lead author Michael Retsky, Ph.D., an investigator in vascular biology at Children's Hospital Boston. "The surprise to us was that the first peak represented patients who actually had their cancers accelerated by surgery."
At the very least, young women should be informed of the phenomenon when they give informed consent, Retsky said.
Dr. Cornelia J. Baines, in a commentary in the Oct. 15, 2004 Journal of the National Cancer Institute, said that the "mortality paradox" would explain the results from the Canadian National Breast Cancer Screening Trial. That trial found screened women between 40 and 49 had 36% more deaths than unscreened women. Critics argued that the Canadian study's methodology was flawed, the increase in mortality was not statistically significant, and the mortality rate was not consistent across individual studies.
Baines, a professor emeritus of public affairs at the University of Toronto, said that the increase in cancer could be attributed to stimulation of dormant metastases by surgery or by the low-energy x-rays used in screening mammography. The final word may have to await results this year from a U.K. trial that recruited women to be screened as they turned 40.
The mortality paradox, whether associated with screening or treatment, remains hotly contested. While invasive breast cancer has been observed to grow more quickly in young women than in older women, this is more likely due to a straightforward model of breast cancer growth than to surgery, said Dr. Daniel Kopans, director of breast imaging at Massachusetts General Hospital.
Newsletter
Stay at the forefront of radiology with the Diagnostic Imaging newsletter, delivering the latest news, clinical insights, and imaging advancements for today’s radiologists.













