
Catch up on the top radiology content of the past week.

Catch up on the top radiology content of the past week.
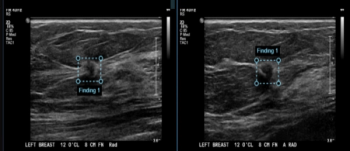
Adjunctive use of an artificial intelligence (AI) software demonstrated nearly equivalent sensitivity and over 28 percent higher accuracy in comparison to radiologist assessment of breast ultrasound images for breast lesions, according to new research presented at the recent Society of Breast Imaging (SBI) conference.

Catch up on the top AI-related news and research from the past month.

Lamenting a lack of control over imaging requests from referring clinicians, this author suggests that a more collaborative approach between referrers and radiologists may facilitate more efficient use of imaging.

Catch up on the top radiology content of the past week.
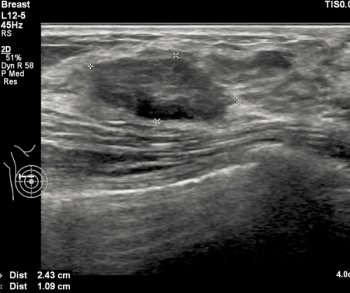
Emerging research shows the adjunctive use of automated breast ultrasound with mammography has similar sensitivity for breast cancer detection as adjunctive handheld ultrasound but may offer reduced false-positive rates in women with dense breasts.

The TE Air reportedly combines enhanced point-of-care ultrasound imaging with an array of practical benefits for radiologists.

Catch up on the top radiology content of the past week.
Is there an optimal pace for navigating the ebbs and flows of our worklists in radiology?

Catch up on the most well-read ultrasound articles from 2022.

Touching on a variety of topics in radiology, here are the top five most well-read articles from Diagnostic Imaging in 2022.

Catch up on the top radiology content of the past week.
In a study of over 800 women with breast cancer, researchers found that African-American women had a higher rate of ductal carcinoma in situ (DCIS) and were less likely to have irregular masses in screening exams in comparison to non-Latina White women.
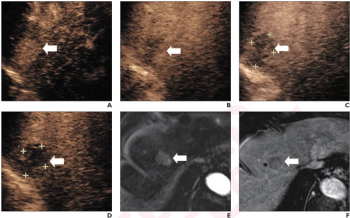
Emerging research showed the combination of contrast-enhanced ultrasound (CEUS) with perfluorobutane and modified 2017 LI-RADS criteria had comparable sensitivity, specificity, and accuracy to current magnetic resonance imaging (MRI) and computed tomography (CT) approaches to detecting hepatocellular carcinoma (HCC) lesions.
The Sonimage MX1 Platinum device reportedly offers a number of features to provide optimal ultrasound image resolution in a variety of point-of -care settings.
In a recent video interview, Thomas Marini, MD discussed the need for ultrasound access to facilitate breast cancer screening in underserved populations and the potential utility of volume sweep imaging, a handheld ultrasound technique that requires minimal training and has a high rate of agreement with conventional ultrasound on BI-RADS assessments.

Catch up on the top AI-related radiology content of the past month.
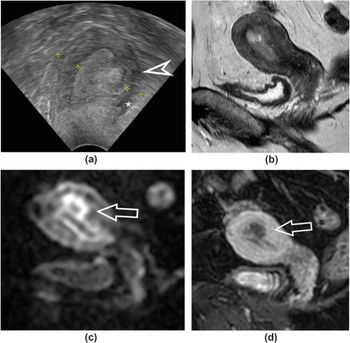
In a new study looking at pre-operative assessment of low-grade endometrial cancer, researchers found that while magnetic resonance imaging (MRI) had 20 percent higher specificity than transvaginal ultrasound for deep myometrial invasion, there was no difference in sensitivity.
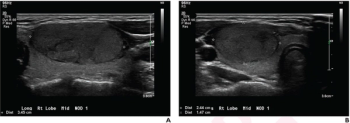
The retrospective study of patients 21 years of age or younger found that a deep learning algorithm and use of the American College of Radiology’s Thyroid Imaging Reporting and Data System (TI-RADS) both had more than a 26 percent greater sensitivity for differentiating thyroid nodules on ultrasound in comparison to radiologist assessment.
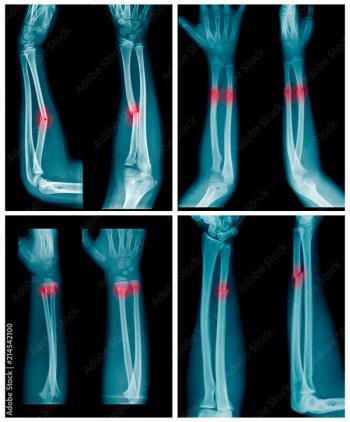
While facilitating interdisciplinary colloaboration is a central objective with enterprise imaging platforms, this author says implementation of these platforms must ensure optimal patient privacy in sensitive cases involving abuse, assault and domestic violence.
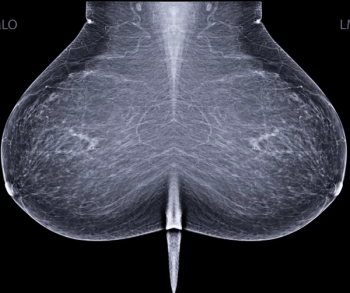
In a recent letter to U.S. Rep. Rosa DeLauro (D-CT), the Food and Drug Administration (FDA) said a final rule on amendments to the Mammography Quality Standards Act (MQSA), including an oft-delayed national standard for breast density notification in mammography reporting, may be published in the next couple of months.

Catch up on the top radiology content of the past week.
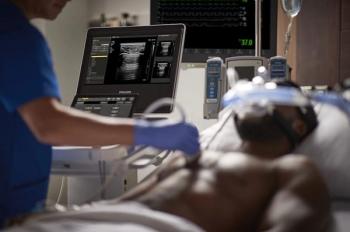
Offering the benefits of real-time collaboration and integrated connectivity, the portable ultrasound device may be utilized in a variety of clinical settings ranging from cardiology to obstetrics and gynecology.
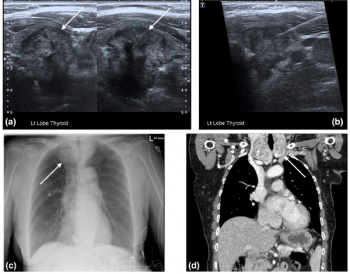
In light of recent shortages of iodinated contrast media, researchers from Australia suggest in a new publication that ultrasound and magnetic resonance imaging (MRI) can be viable first-line imaging options for a number of non-urgent presentations of the head and neck.

The ability of QT Imaging’s QTscan, a quantitative transmission ultrasound modality, to calculate the ratio of fibroglandular volume to total breast volume may facilitate assessment of ongoing breast cancer treatments or selective hormone receptor modulation therapies.